Floré Calprotectin Gut Inflammation Test
Find Out if You Have IBS or IBD
Find out if you have IBS or IBD with our Calprotectin Gut Inflammation Test.
What is calprotectin?
Calprotectin is a protein that is found in bodily fluids and helps aid in the diagnosis of inflammatory bowel disease (IBD).
You should take this test if you’re suffering from*:
- Chronic and constant abdominal pain
- Constipation/Diarrhea
- Mucus in Stool
- Gassiness or Bloating
- Nausea
IBD is classified as a disease whereas IBS is classified as a syndrome. IBS does not cause inflammation and rarely requires hospitalization, but IBD can cause destructive inflammation and permanent damage to the intestines. IBD also increases your risk for colon cancer, IBS does not.
*symptoms indicated by crohnscolitisfoundation.org
What is the Floré Calprotectin Gut Inflammation Test?
Diagnoses inflammation within your gut through the quantitative measurement of fecal calprotectin in your stool. This test aids in the diagnosis of inflammatory bowel disease (IBD), specifically Crohn's disease (CD) and ulcerative colitis (UC) and can help differentiate IBD from irritable bowel syndrome (IBS), in conjunction with other laboratory and clinical findings.
Inflammatory Bowel Disease (IBD)
Irritable Bowel Syndrome (IBS)
Ulcerative Colitis (UC)
Crohn's Disease (CD)
The Fastest, Most Accurate Diagnosis Tool for Gut Inflammation

Get Your Results in as Little as 3 Days

The Highest Level of Accuracy

Differentiates Between IBS and IBD
The Process
Your Sample Analysis
Our test is a colorimetric, microtiter plate-based enzyme linked immuno-sorbent assay that uses monoclonal antibodies (mAb) highly specific to calprotectin.
Review Results
Results will be uploaded to our portal and available for review by you and your provider.

How Does It Work?
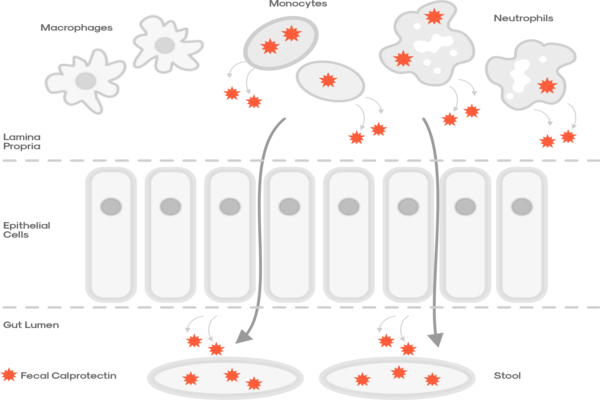
Differentiating Between IBS and IBD
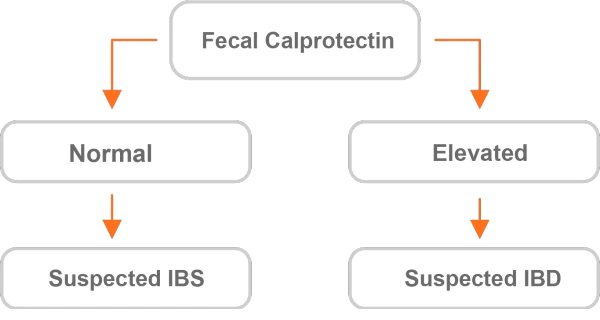
- Test results should be interpreted in conjunction with information available from clinical assessment of the patient and other diagnostic procedures.
- Fecal calprotectin results may not be clinically applicable to children less than 4 years of age.
- Patients taking non-steroidal anti-inflammatory drugs (NSAID) may have elevated fecal calprotectin levels.
- Patients with granulocytopenia may have false negative results due to bone marrow depression.
- Patients with IBD fluctuate between active (inflammatory) and inactive stages of the disease. These stages must be considered when interpreting results of the fecal calprotectin assay.
